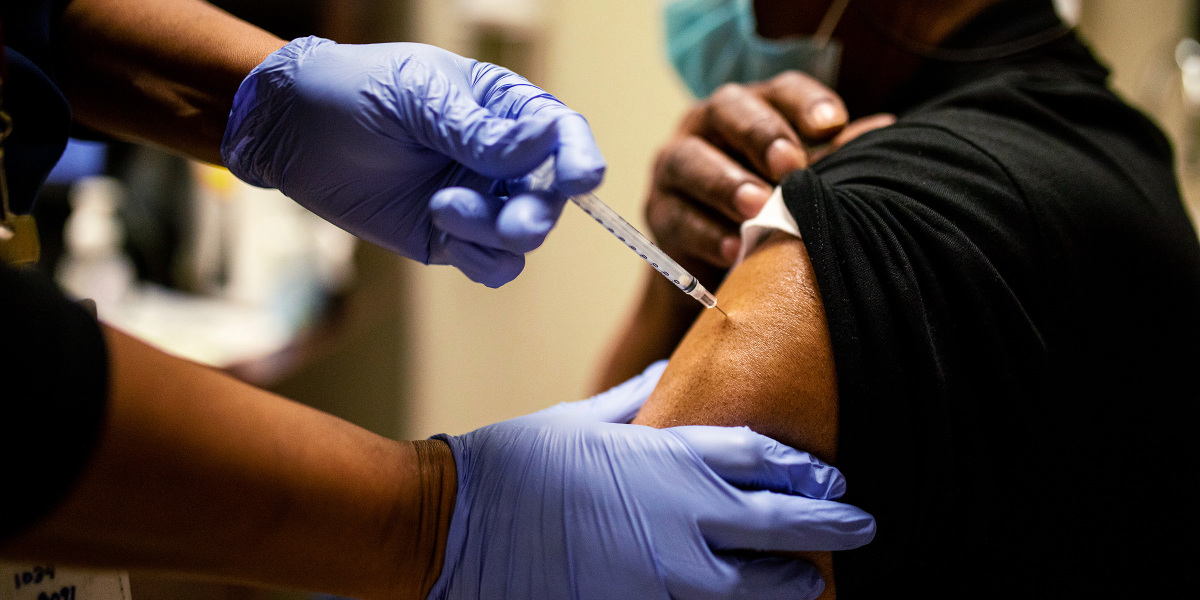
“The problem right now is that it’s being talked about so much as a choice,” says Brunson, who points out that white Republican-voting men are particularly reluctant to get vaccinated relative to the rest of the US population. “Focusing on things that are choices takes away the spotlight from really severe access issues in the US.”
One success story took place in Philadelphia, thanks to an effective collaboration between two health systems and Black community leaders. Recognizing that the largely online signup process was hard for older people or those without internet access, Penn Medicine and Mercy Catholic Medical Center created a text-message-based signup system as well as a 24/7 interactive voice recording option that could be used from a land line, with doctors answering patients’ questions before appointments. Working with community leaders, the program held its first clinic at a church and vaccinated 550 people.
“We’ve worked really closely with community leaders, and every clinic since has evolved in terms of design,” says Lauren Hahn, innovation manager at the Penn Medicine Center for Digital Health.
By including community members early on, Hahn hoped, the program would give the people coming in for their shot the feeling that the clinic was made for them. And after their appointment, patients were sent home with resources like the number for a help line they could call if they had any questions about side effects.
“We want to make sure that we’re not just coming in and offering this service and then walking away,” she says.
Data needs to guide practice
Researchers say that having complete data on who is—and isn’t—getting vaccinated can improve the vaccine rollout and prevent problems from being obscured. Data gaps have been a problem since the early days of the pandemic, when few states were reporting cases and deaths by race. Though Joe Biden has emphasized equitable vaccine distribution as a priority, the CDC reports having race and ethnicity data for only 56.7% of vaccinated people.
Not everyone wants more information to be made public, however. In Wisconsin, Milwaukee County executive David Crowley says there can be resistance to collecting and publishing data that shows disparate health outcomes among racial groups. “We have to say that racism has been a problem,” Crowley says. But, he adds, “Look at the data. It’s going to tell you a story right there.”
His county created a covid-19 dashboard that reported detailed racial data before many other jurisdictions in the state, Crowley says. It allowed the county to work with the city of Milwaukee to open special walk-in sites for residents in certain zip codes.
“We haven’t found the silver bullet in all of this,” Crowley says. “But at the end of the day, we know that data is telling a story, and we have to utilize this data.”
“Covid is what really catalyzed this type of analysis work.”
Dan Pojar, Milwaukee County EMS
Because the data is public, other pandemic response teams outside of government could use it too. Benjamin Weston, director of medical services at the Milwaukee County Office of Emergency Management, says making covid-19 data transparent and accessible helped community groups and academic researchers know where to focus their efforts.
The dashboard has also helped them see, in stark terms, that the communities hit hardest by covid have historically faced broader health challenges. After seeing that covid rates were high in places where people typically have cardiac issues, for example, the county decided to offer CPR training at covid vaccination sites. EMS division director Dan Pojar says he expects about 10,000 people to get CPR training that way.
“That’s an opportunity for us to work with other health systems to flow education and different initiatives into these communities,” Pojar says. “Covid is what really catalyzed this type of analysis work.”
It might get harder from here, not easier
Public health and equity researchers were not surprised at the pandemic’s disparate effect on certain communities, according to Stephanie McClure, assistant professor of anthropology at the University of Alabama. Health disparities along racial and economic lines have the potential to become a national and local focal point—in April, CDC director Rochelle Walensky declared racism “a serious public health threat”—but that tide hasn’t yet turned, McClure says.



Recent Comments