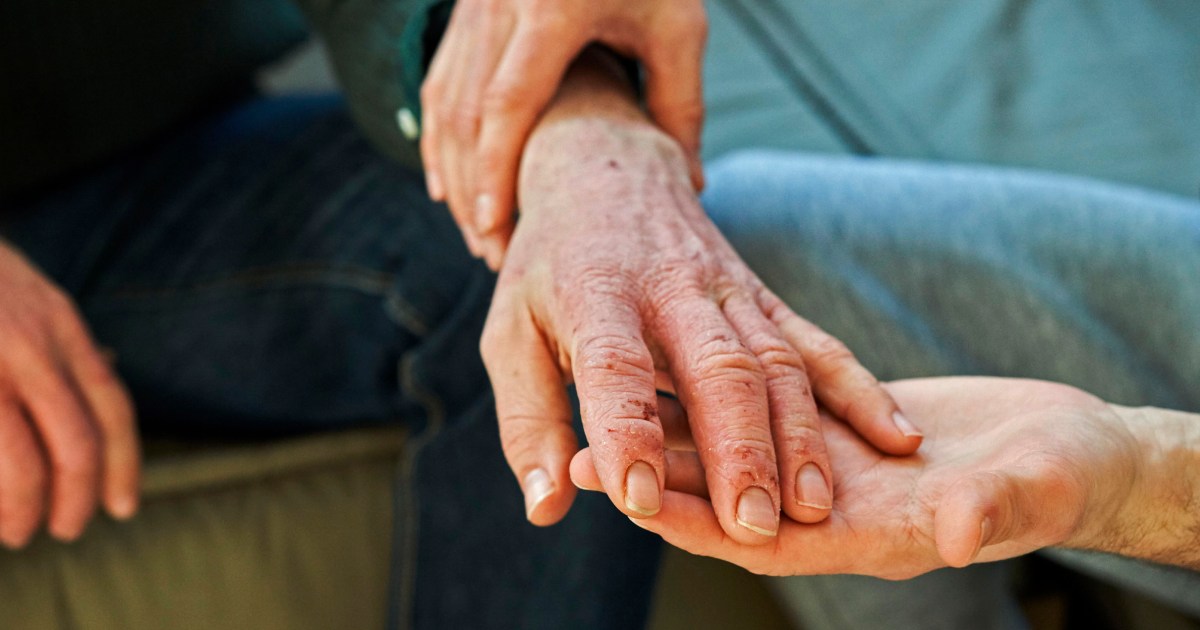
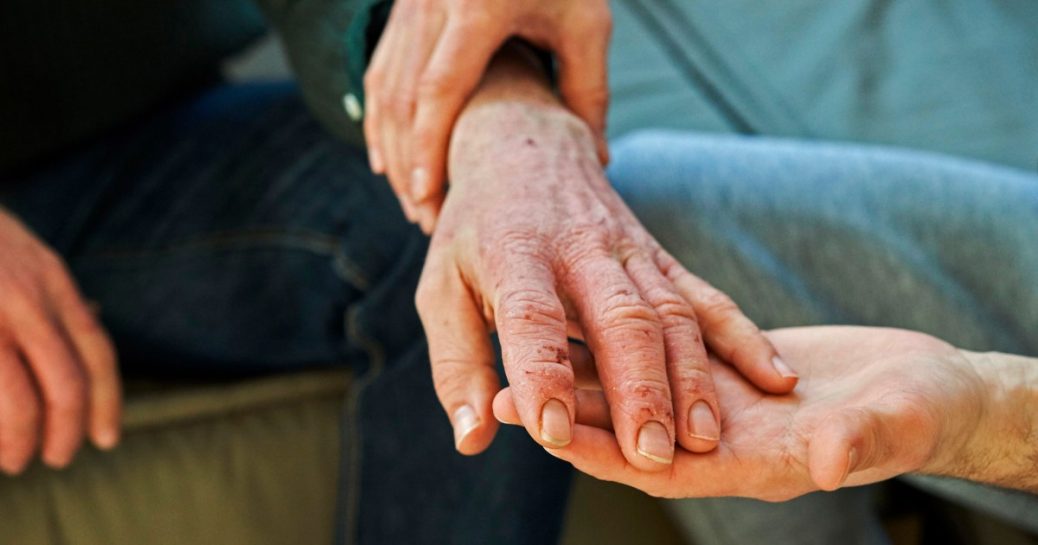
Scientists are still unraveling the mystery of why skin conditions like eczema cause people to itch.
One known cause is inflammation, which gets worse as people scratch and their skin becomes damaged. But there may be another trigger for itchiness, according to a study published Wednesday in the journal Cell: a bacterium called Staphylococcus aureus.
Researchers from Harvard Medical School found that the bacterium can directly activate nerve cells in mice.
“What was surprising is that in some situations where there was very little inflammation, we could still see the mice scratching. It turns out, the reason is that the bacteria was directly acting on nerve fibers that produce itch,” said a co-author of the study, Isaac Chiu, an associate professor of immunology at Harvard Medical School.
Before the study, scientists were aware that S. aureus was associated with eczema, but the exact link was unclear. The new research found that once S. aureus invades a mouse’s skin, it releases an enzyme called V8. That, in turn, activates a protein called PAR1, which is located on nerve cells in the skin. The activated protein sends a signal to the brain that makes the mouse itchy — and prompts it to start scratching.
Lab experiments involving human nerve cells showed the same mechanism is possible in people, but the researchers aren’t sure yet whether the findings directly translate.
Still, the research may offer scientists a new direction to pursue in developing treatments for eczema, which affects around 10% of people in the U.S. The most common type, atopic dermatitis, causes chronic itchy and dry and cracked skin, and it is strongly associated with allergies such as asthma or hay fever.
“For patients with atopic dermatitis, almost all of their lesions harbor Staph aureus,” said another co-author of the study, Liwen Deng, a postdoctoral researcher in Chiu’s lab.
In the study, mice were exposed to S. aureus bacteria directly on the skin for several days. By the third day, the researchers found, the animals developed skin irritation, then significantly increased scratching by the fifth day compared to mice who weren’t exposed to the bacteria.
The affected mice were also more likely to develop alloknesis — a condition in which people itch from triggers that don’t normally cause itching, like a gentle touch.
To rule out the possibility that inflammation might still be driving the itch response, the research also involved mice that had lower levels of immune cells or inflammatory chemicals associated with skin allergies. The results still suggested that the bacterium was the cause of the itchiness.
“Their study was able to break apart the inflammatory response and the itch response,” said Nathan Archer, an assistant professor of dermatology at Johns Hopkins University School of Medicine, who wasn’t involved in the research.
Dr. Peter Lio, the founding director of the Chicago Integrative Eczema Center, said in an email that the Harvard study “strengthens and furthers our understanding” of the role Staph bacteria play in itching sensations.
“We have learned about the many toxins that Staph expresses: some drive inflammation, others drive skin barrier damage and others directly drive itch,” said Lio, who also wasn’t involved in the research.
Archer said the study could offer important clues about how to treat patients with eczema who don’t respond to available treatments. Doctors commonly prescribe topical steroids, and an injection for adults with moderate or severe eczema was approved in 2017.
Deng said, “Right now there aren’t really targeted treatments to go after bacteria.”
In the future, she said, scientists might be able to develop a topical treatment that blocks the S. aureus pathway that leads to itchiness. Another option would be to repurpose an anti-clotting medication called Vorapaxar to treat eczema, because, she said, it’s the only drug approved by the Food and Drug Administration that blocks the PAR1 protein.
In the new study, Vorapaxar seemed to reduce the desire to scratch in mice who received it.
Chiu said the research might even have applications for skin conditions beyond eczema, such as impetigo, an infection that causes red facial sores in infants and children.
“Any situation where there might be Staph aureus present on the skin could be relevant to our findings,” he said.








Recent Comments