As a third surge of the coronavirus threatens much of the United States, public health experts across the country say there still aren’t enough tests available to keep the virus under control.
Right now, some doctors and hospitals are offering rapid tests to patients, which can give results in minutes. And over the next few weeks, major pharmacy retailers like CVS and Walgreens say they’ll start offering a type of rapid test called an antigen test, which some hope will give Americans more access to testing.
Full coverage of the coronavirus outbreak
“There’s a need for testing across the board,” Gigi Kwik Gronvall, senior scholar at the Johns Hopkins Center for Health Security, told NBC News.
About 30 million Covid-19 tests are given every month, according to estimates from The Atlantic magazine’s Covid Tracking Project. But studies have found that the U.S. would need millions more —193 million a month, according to one report — to be effective.
One major issue has been a shortage of crucial testing supplies that’s been plaguing labs since the start of the pandemic.
“The supply chain hasn’t met the demand,” said Dr. Patrick Godbey, president of the College of American Pathologists. “We still cannot get enough reagents to perform the tests we would like to perform. It’s not just testing reagents, but supplies like swabs.”
In response, the federal government is pushing rapid or point-of-care testing, as opposed to the gold standard polymerase chain reaction, or PCR test, which requires samples to be sent to a lab for analysis and can take days to come back.
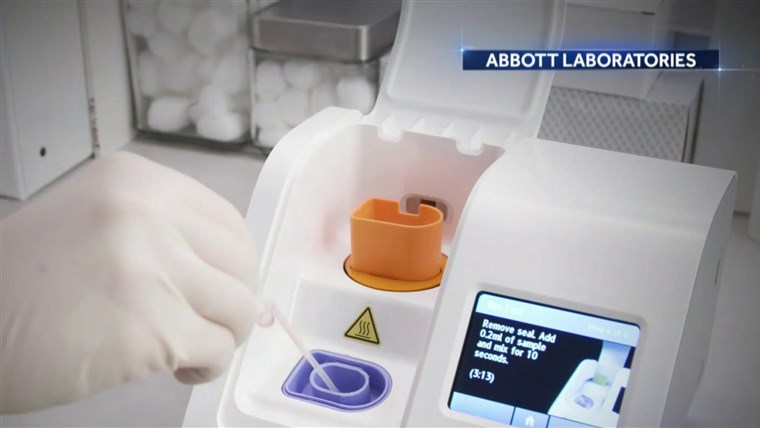
Two weeks ago, the Department of Health and Human Services started sending states rapid antigen tests made by Abbott Labs. The test is the simplest to date because it doesn’t require a machine and results take about 15 minutes. Some state health officials told NBC News that the tests will be used in nursing homes and schools.
“In general, I say that it’s a good start,” Dr. Michael Mina, an epidemiologist at Harvard T.H. Chan School of Public Health, said Friday on a call with journalists. “But I’m extraordinarily frustrated that the federal government is just continuing this position where their only strategy is to purchase what becomes available through industry and corporations in the private market.”
“Different places need different types of tests,” Gronvall said. “The most important feature is the speed at which you can deliver accurate results.”
But accuracy has been the thorn in the side of rapid testing, as witnessed this month when nearly 20 members of the Trump administration and campaign, including the president and first lady, became infected with the virus. All staff members and visitors to the White House were said to be undergoing regular rapid testing to screen for Covid-19.
The problem is that rapid tests aren’t as sensitive as PCR tests, with as many as 1 in 4 results being false negatives.
About a dozen rapid tests have been granted emergency use authorization by the Food and Drug Administration. All of them are meant for patients who are experiencing symptoms, because that’s when they have higher levels of virus in their bodies.
“The point-of-care tests have their place and that needs to be defined by the individual situation,” Godbey said. “You’re in the doctor’s office and you come in and have a fever, along with symptoms that began five to seven days ago. The rapid test has a place there.”
Download the NBC News app for full coverage of the coronavirus outbreak
But the fear is that as these tests become more widely available, they could be used as a screening tool, similar to what the White House is doing, a method that backfired after guests at a Rose Garden event last month were told they didn’t need to wear masks after getting a negative rapid test result. At least a dozen of those guests ended up getting sick with the virus.
“Negative results should not be viewed as a guarantee of negativity or safety,” said Dr. Christopher Polage, director of the clinical microbiology laboratory at the Duke University Health System.
A new study that looked at Abbott’s antigen test, called BinaxNow, found that it could work as a complement to PCR testing. While the study was small and results have not yet been published or peer-reviewed, researchers at the University of California, San Francisco, found that of 26 people who tested positive on a PCR test, 15 of them were also identified on Abbott’s test. But researchers point out, those 15 were the most infectious because they also had a high amount of virus in their samples. Nearly half of those 15 were asymptomatic.
“Breaking the back of this pandemic can be accelerated if we could deploy and act on a rapid test that detects the persons who are most infectious and require isolation, many of whom may be asymptomatic,” study author Dr. Diane Havlir said in a news release. “PCR remains the gold standard, but a strategic combination of these tests could assist in public health settings where rapid results and knowledge of transmission risk on the day of testing are critical.”
Follow NBC HEALTH on Twitter & Facebook.
Akshay Syal contributed.








Recent Comments