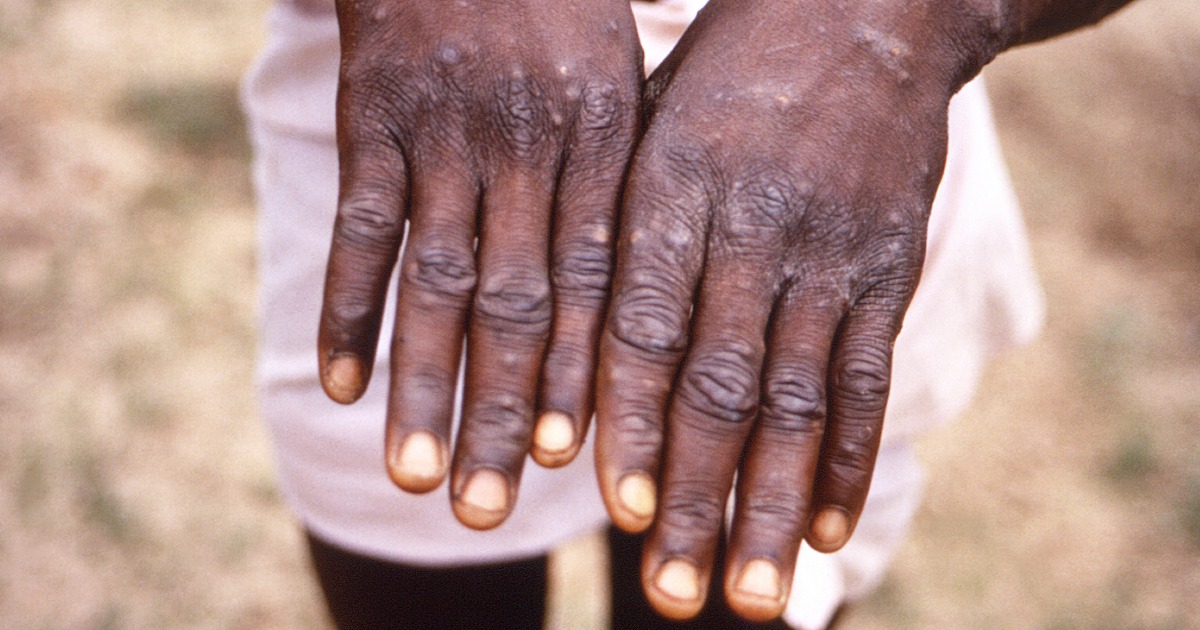
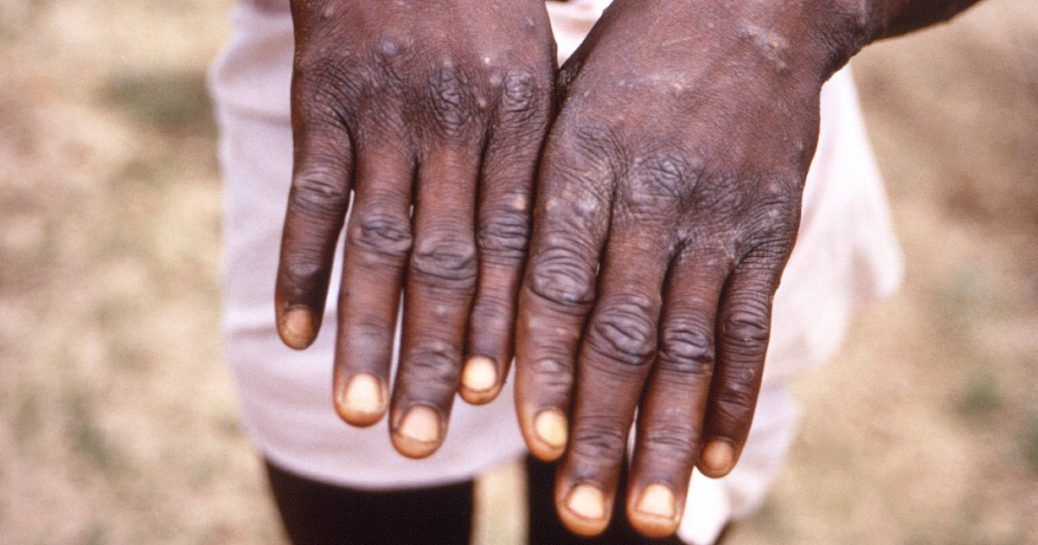
In a matter of weeks, around 80 new cases of monkeypox have been reported across eight European countries, an unprecedented outbreak of a disease that rarely spreads outside central and western Africa. A handful of additional cases have been reported in the U.S., Canada and Australia since Wednesday.
The growing case tally has raised questions among disease experts about the nature of monkeypox’s transmission, since many of the patients have no history of travel to Africa or known exposure to an infected person.
“How they initially got infected and why it’s all over the place is still a mystery,” said Dr. Stuart Isaacs, an associate professor of medicine at the University of Pennsylvania.
Monkeypox doesn’t easily jump from person to person. Until now, most infections occurred among people who’d been exposed to an infected animal through bites, scratches or the preparation of meat from wild game, experts said. The most notable outbreak in the Western Hemisphere occurred in 2003, when pet prairie dogs infected 47 people in the U.S.
From past instances of human-to-human transmission, scientists have learned that the virus spreads through the exchange of large respiratory droplets or via direct contact with bodily fluids, lesions that form during infection, or contaminated items like clothing or bedding. Monkeypox isn’t considered a sexually transmitted infection, but it could be passed during sexual encounters, experts said.
Many of the recent cases in Europe are among men who have sex with men, and a Friday alert from the Centers for Disease Control and Prevention suggested that some recent cases started out with lesions around the anus and genitals.
“I’m guessing that sexual transmission will be high on the list of potential culprits,” said Dr. Grant McFadden, director of the Biodesign Center for Immunotherapy, Vaccines and Virotherapy at Arizona State University.
McFadden, Isaacs and several other experts offered their early ideas about to how and why the new outbreak has swelled.
McFadden said the genetic sequence of the monkeypox virus that has infected people in Europe looks relatively run-of-the-mill. That’s a clue that human behavior, rather than inherent changes in the virus itself, might be driving the new cases.
“It could be just a simple, accidental chain, for example, into the gay community,” McFadden said.
Viruses often transmit more easily within tight-knit groups of people. According to Global.health, a group that gathers infectious disease data, all of the recent monkeypox cases for which gender has been reported have been male.
“You could imagine one person had it and, if they’re part of a small, intimate group of people, could have spread it amongst those connections,” said Dr. David Evans, a virologist at the University of Alberta.
But that doesn’t explain why the cases are so geographically dispersed. And the experts also agreed that it’s premature to suggest monkeypox is solely spreading within any one community. It will be important to pinpoint the first case of human-to-human transmission and study it, they said, to determine how the outbreak started.
Some experts hypothesized that the loosening of international travel restrictions may have contributed to the spread.
“It kind of looks like the virus always had this potential capacity” for human-to-human transmission, McFadden said. “It just never had the opportunity in the past — or if it did, it quickly petered out and we never really saw it as an event. Whereas now with people being able to travel all over the world, it’s entirely possible we’re actually seeing it for the first time in a larger context.”
People may be more susceptible to monkeypox now than in the past
Most people who get monkeypox make full recoveries. In the past, just 1 percent of people who’ve gotten the West African strain responsible for the new outbreak have died. But a different lineage of the virus, the Congo Basin clade, has killed closer to 10 percent, according to the World Health Organization.
Monkeypox belongs to the poxvirus family, which includes smallpox. Smallpox vaccines are around 85 percent effective at preventing monkeypox, the WHO estimates. But the U.S. stopped vaccinating the public for smallpox in 1972, and global vaccination ceased around 1980, when smallpox was eradicated worldwide.
So people have less immunity to poxviruses overall than in decades past.
“We no longer have immunity and therefore we’re going to continue to see cases emerge — and more of them over time,” said Anne Rimoin, an epidemiology professor at the University of California, Los Angeles Fielding School of Public Health.
Isaac said diminished population immunity could also explain why Africa has recorded more monkeypox cases in recent years. The Democratic Republic of the Congo reported up to 18,000 confirmed or suspected monkeypox cases from 2010 to 2019, but fewer than 10,000 between 2000 and 2009. In 2020 alone, the country reported more than 6,000 suspected cases, according to the WHO.
Doctors may have missed some early cases
Monkeypox may have started spreading in Europe a while before it landed on scientists’ radars, several experts suggested.
“Because of the geographically dispersed nature of the cases across Europe and beyond, this suggests that transmission may have been ongoing for some time,” Dr. Hans Kluge, WHO Regional Director for Europe, said in a statement on Friday.
Isaacs said doctors can sometimes miss a monkeypox case because the rash looks similar to chickenpox, syphilis or herpes.
“Most doctors and clinics are not thinking about monkeypox,” he said. “It may have been brewing over time and just no one thought to identify or think about this.”
That’s especially likely if a patient has mild disease, McFadden said. So far, that’s been the case among most of the new infections, according to reports from the U.S., Belgium, Canada, Germany and Portugal. No recent deaths have been reported.
“If it was particularly mild, someone may not really have really noticed much and didn’t think much of what was going on and then spread it amongst their their social group,” Evans said.







Recent Comments